Health Fair Planning Guide – Health Fair Activities – Health Fair Banner
Freebie Alert! This post is packed with free health fair activity ideas, free health fair handouts, and free health fair planning resources. Use it to make your next health fair or wellness fair a success.
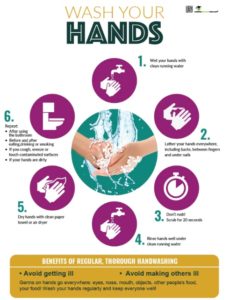
Cheryl Bachinski, a school nurse, is planning a health fair and she needs a banner to help people who are constrained by time and money to make better choices for their families who are struggling with their weight. She says they drink too many sweetened sodas, eat too many cupcakes and chips, along with other packaged snacks, and they never exercise. Wait until you see the new banner we created for her. Check it out and you can buy it on sale or use the display idea for your own.

How will you stand out from the crowd at the next health or wellness fair?
Ready for the answer?
It’s all about the booth.
Yes, there are totally committees, special presentations, and deals with vendors, but in our experience, a successful day at a health fair comes down to your booth.
So, that’s what we’re going to address — tips and tricks for putting together the best nutrition education wellness fair booth around.
Objectives:

Wellness and Health Fair Kit
Let’s begin by setting up some objectives for your day at the health fair. Which of the following is an objective you’d like to address? Does the health fair have a preexisting theme?
- Health awareness
- Health screenings
- Immunizations
- Marketing
- Community event
If more than one objective applies to you, great! However, if all of them apply to you, you may want to narrow your focus to just 1 or 2 primary objectives that you can use your booth to address.
Resources:
When it comes to big events that require committees and multiple vendors, there are lots of resources to make life easier. Look through the following guides if you’re putting together your own large health fair or wellness event…
Now, back to the booths.
Use our new handy theme-picker to choose the theme that is right for you or read below for more ideas.
Theme Ideas for Children:

Wellness and Health Fair Kit for Kids
If your health fair booth is geared towards children, you will have the best results with simple, colorful, and engaging content. Coming up with those materials and then coordinating them will get a lot easier if you select a single theme for your booth. Some of the most popular themes that we’ve used or observed (and can therefore recommend to you) include…
Theme Ideas for Adults and Older Kids:

Salsa Wellness Fair Kit
Most wellness fairs appear to be geared towards adults these days, so if that’s what you’re working with, consider any of the following tried-and-true themes…
Theme Ideas for Families:
There are many ways that families can team up to improve their health together, but most people suffer from a crisis of imagination and can’t think of a way to implement a healthful habit as a family. Inspire them with these wonderful family-friendly health and nutrition themes.
Building a Great Booth and Activity Center:
So, once you have an overarching objective identified and a theme established, it’s time to get down to business.
Your booth.

Make Your Salad a Rainbow Banner
How can you make it engaging, with activities that draw and hold participants?
Establishing a theme was a great start. So was finding an objective. Use these to guide the nitty-gritty of your booth.
Based on the wellness fair we have participated in, observed, and/or discussed, the most successful booths have balanced a combination of the following…
- Engaging banner
- Interactive component
- Giveaway
- Resources for more information
If you don’t have space or resources for all four, pick as many as are reasonable and build your balance from there.
So, first up, the banner. There’s a comprehensive post about wellness fair displays, and it has everything you need to know about banners. Of course, you can also save yourself the headache (and multiple trips to the store for supplies) by buying a crowd-tested, scientifically-accurate, and utterly up-to-date banner that matches your vision for the booth.
Next we’re going to tackle the interactive component. Just kidding. We’re going to go really in-depth with that one, so it gets its own section further down. Stay tuned!

Real Food Grows Bookmark
The third element of an engaging wellness fair booth is a giveaway. You can either set up a raffle for a large prize or offer a selection of smaller prizes. Great prize ideas include…
- Cookbooks
- Bookmarks
- App download codes
- Recipe cards
- Cooking utensils
- Exercise equipment (like jump ropes, hula hoops, etc)
You know your audience. What resonates the most with them?
So. Why a giveaway? A giveaway will draw people to your booth, especially if you offer unique prizes and get the word out about your raffle or treat. Once people are at your booth, you can convey the messages that you want to communicate. It’s hard to get the word out if no one comes to your booth!
The final element of a successful wellness fair booth and/or activity center is a way to offer your audience more information. Often people would like to learn more about a topic at their leisure, rather than while standing in the middle of a busy nutrition fair. Handouts, lists of helpful websites, reference materials, or recipe cards are all great resources to have at your booth. That way, people can revisit the keys of your message, making it more likely to stick in their minds.
Great Wellness Fair Activity Ideas:

Prevent the Flu Poster
The interactive component for a wellness fair can be adjusted to fit your space, resources, and audience. Consider…
- Having passers-by participate in an activity or game (examples below)
- Setting out food samples. Especially if you’re putting together a healthful cooking or balanced lifestyle booth, little samples of healthful foods to sample (with recipes to match) can be a big hit at wellness fairs. You can also include a survey or do a taste test to have people evaluate different healthful foods.
- Giving cooking demonstrations.
- Surveying your audience about their health, habits, goals, etc.
- Taking health readings. Offer the resources for participants to measure their BMI, waist circumference, blood pressure, etc. Follow-up materials here are a must.
So, want to do an activity? Here are some examples of our favorite health and wellness fair games…
Activity #1: MyPlate Trivia
Divide participants into balanced teams and bring on the trivia. The first team to answer each question correctly will earn a point, and the team with the most points at the end of the game wins.
Question #1: How much of your plate should be filled with fruits and vegetables at each meal?
Answer: Half
Question #2: What should you drink instead of sugary drinks?
Answer: Water or skim milk
Question #3: What are the five main MyPlate food groups?
Answer: Fruits, Vegetables, Grains, Protein, and Dairy
This activity idea offers the perfect way to merge the activity and giveaway elements of your booth. Offer prizes to all participants, or just to the winning team (if you want to incentivize engagement). In lieu of smaller prizes, you can also give away raffle tickets for one of your larger items.
Activity #2: Heart Health Taste Tests

About Your Blood Pressure Poster
Eating well for your heart doesn’t mean giving up all of your favorite foods to go on a taste-free diet, but some clients and patients don’t really understand that point. Bring the lesson home by having a taste test session right at your booth with some of your favorite heart-healthy products or recipes.
Consider a trans-fat-free margarine tasting, for example. Just bring in margarines that contain less than 2 grams of saturated fat and 0 grams of trans fat per serving. Have people who wander by your booth try these items, preferably spread on a bit of whole wheat bread or on a whole grain cracker.
You can also do taste tests with salads that feature veggies that are especially high in fiber, or with various types of quick-cooking oatmeal for a heart-healthy breakfast. You can tailor your tastings to fit the budget and equipment that you have.
Activity #3: What’s the Link?
This activity can be adapted to any theme you’d like. We’re going to outline it with an example — in this case, high-fiber foods.
Display beans, oatmeal, apples, brown rice, canned peas, shredded wheat and whole grain bread (and other high-fiber foods). The question for the display should be, “What do these foods have in common?” The answer of course, is “fiber”! Anyone who guesses correctly can receive a raffle ticket that is good towards a free prize — or a first look at the smaller prizes laid out on the table.

MyPlate Poster
Amazing Handouts for Wellness Fairs:
No wellness or health fair booth would be complete without a handout or five. These can be woven into your display or photocopied and laid out in stacks for people to take home. Today, because it’s Nutrition Month, and because we love you, here are links to 5 amazing and totally free handouts that you can use at your booth.
Want a hand getting started? Download this free health fair planning checklist today! This organizational checklist will help you efficient and make the best health fair.
And the best part?
It’s totally free!

Good luck with your health and wellness fair!